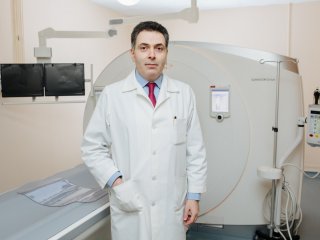
We discussed long COVID, its manifestations, and treatment with Corresponding Member of the Russian Academy of Sciences, Deputy Director of Lomonosov Moscow State University Medical Center Simon Matskeplishvili. The famous cardiologist spoke about the link between coronavirus and cardiovascular diseases.
— What have we recently learned about the coronavirus?
— The General Meeting of the Russian Academy of Sciences opens tomorrow, dedicated to the most relevant topic to date — the COVID-19 pandemic, which has radically changed the usual course of things. On the one hand, this is a serious challenge to all of humanity, and on the other hand, we have witnessed breakthrough scientific research and discoveries in biomedicine. I’m sure that such unprecedented progress will change the vector of development of medical science as a whole and will not only allow us to cope with the pandemic soon, but will also lead to the emergence of innovative, effective, and, most importantly, affordable methods of treatment of cardiovascular, oncological and many other diseases.
It is encouraging to see how the status of a scientist in the modern world is changing and growing before our eyes. Many people of completely different specialties are involved in the fight against the pandemic, but it is the science that has proved to all of us that it provides the ability to withstand the most difficult problems and solve the most important tasks that nature and life face us. It is obvious that great attention must be paid to science on a global scale.
We see such unique achievements of Russian scientists as the development and creation of COVID-19 vaccines, the synthesis of monoclonal antibodies that can both protect against the disease and treat it, as just a few weeks ago, the scientific director of the Engelhardt Institute of Molecular Biology, Member of the Russian Academy of Sciences A.A. Makarov reported to the President of the Russian Federation.
Moscow State University has also taken and continues to take an active part in the fight against COVID-19. We are engaged both in the treatment of patients based on the unique protocol of the MSU Medical Center, which has demonstrated its effectiveness and safety, and conduct serious interdisciplinary world-class research in this area. Now we are focused on the treatment of long COVID. I would like to note that the number of such patients is increasing like an avalanche.
— How often do you, as a cardiologist, face the long-term consequences of COVID? When, for example, a person got sick, and six months later suddenly starts having serious heart problems.
— This is a very important question. Such patients come literally every day. I cannot but note that there is an important difference between the treatment of long covid and rehabilitation after COVID-19: it is not the same thing, although these concepts are often confused with each other. Let me remind you that according to the International Classification of Diseases (ICD-10), long COVID is a condition in which complaints and symptoms in patients develop during or after COVID-19, last for 12 weeks or more, and are not the result of another disease.
There is a significant number of people who cannot recover after several months, and sometimes the state of ill health remains even for a year and a half. The acute period is over, the coronavirus is not detected in tests, there are no pronounced inflammatory changes in blood tests, radiological diagnostics also does not reveal serious problems, but the general condition and quality of life suffer significantly, and whole catalogs have already been published in terms of the number and variety of complaints.
— What are these complaints about?
— Patients complain of ailments associated with impaired activity of the nervous, musculoskeletal, respiratory, cardiovascular, digestive, and other systems. These are sleep disorders, prolonged loss of sense of smell and phantom odors, memory lapses, bad mood, depression, muscle pain, fatigue, exercise intolerance, shortness of breath, and much more.
Separately, I would like to highlight the cardiovascular manifestations of long COVID. From my point of view (and this is confirmed by the specifics of the pathogenesis of the disease and its clinical picture), the main target of COVID-19 is the circulatory system: heart, blood vessels, blood clotting system. The cardiovascular system is damaged both due to the direct cytotoxic effect of the coronavirus, which can infect both heart muscle cells and vascular endothelial cells, and, to a greater extent, by the immune system. A feature of the SARS-CoV-2 virus is also the ability to bind firmly to a specific spike protein receptor – angiotensin-converting enzyme 2 – which leads to significant inhibition of its activity. ACE2 is located on cell membranes and in blood plasma, it has several important functions, one of which is the degradation of angiotensin II, the accumulation of which, in turn, causes spasm of small blood vessels, activation of the blood clotting system with the development of multiple thromboses, inflammation of the blood vessel wall, tissue fibrosis. Such multiple lesions of the circulatory system during acute COVID-19 lead to severe disruption of blood supply to almost all organs and tissues of the body and are one of the leading causes of complications and undesirable outcomes of the disease, including fatal ones.
We see the long-term consequences of this process in the form of a number of cardiac manifestations of long COVID: arrhythmias, palpitations, inflammatory myocardial diseases (in a small percentage of cases), exacerbation of cardiovascular diseases – arterial hypertension, coronary heart disease, heart failure.
Doctors take this problem very seriously. Within the framework of an international group of scientists, which includes the world’s leading cardiologists, we formulated, described, and proposed to identify a new clinical phenotype of long COVID – post-COVID-19 tachycardia syndrome – as an independent condition after acute COVID-19. We consider the heart rate as an integral indicator of the state of the autonomic nervous system, the violation of the activity of which underlies most of the manifestations of long COVID. It is also important that the heart rate is an easily measurable, objective quantitative parameter. So, we get a completely accurate indicator that can be easily monitored, and by the dynamics of which we can track the patient’s condition as a whole.
Today we are already beginning to understand the cause and mechanisms of post-COVID-19 tachycardia and are developing a protocol for the treatment of this form of long COVID. This work, in particular, is carried out jointly with colleagues from the Karolinska Institute in Stockholm, the Federal University of Rio de Janeiro, the Charité University Hospital in Berlin, the University of California in San Diego.
Unlike rehabilitation after disease, the treatment regimen being developed will include drugs of several pharmacological groups aimed at restoring disorders of the cardiovascular and nervous systems. We hope that such an approach will preserve health and ensure a normal quality of life for many patients with long COVID. Taking into account the hundreds of millions of reported cases of the disease, helping such patients will become the most important task of healthcare worldwide.
Deputy Director of Lomonosov Moscow State University Medical Center Simon Matskeplishvili. Photo: Nikolay Malakhin / Scientific Russia
— Is there a correlation with age: the older a person is, the more pronounced long COVID?
— In fact, no. I would say that there is rather a correlation with the severity of COVID-19, and often it is even the opposite: the more severe the disease is, the more the immune system is activated, the more complete, if I may say so, recovery with a fairly small number of long-term consequences. Yes, it may take a long time for such patients to get out of the disease, often up to three weeks or more, but severe asthenia in the period of convalescence should not be confused with long COVID, which we observe three or more months after the disease.
If a person has a mild form of the disease, without high fever, respiratory failure, a significant increase in the level of inflammatory blood parameters, etc., then, though it may seem strange, they are more susceptible to the development of long COVID.
— And what is known about T-cell immunity, which is believed to play a crucial role in protecting against COVID-19?
— T-lymphocytes and many of their subpopulations, which interact with foreign antigens through their own receptors and destroy the cells with which they are associated (in this case, cells infected with a virus), are the main link of antiviral immunity. Immunoglobulins, or antibodies, which are synthesized by B lymphocytes and provide humoral immunity, mainly bind to virus antigens (primarily spike protein) and prevent their interaction with specific receptors, in the case of SARS-CoV-2 – with angiotensin-converting enzyme 2. The memory of a viral infection is preserved in the form of memory cells of both T-cell and B-cell immunity.
Even though today there are quite many ways to determine the intensity of T-cell immunity, this is a rather complex technique. From the point of view of science, of course, it is very important and will definitely be studied, but from the point of view of practical application, I think it will not be used routinely. In medicine, there is such a principle: any diagnostic test should be performed only if further examination or treatment of the patient depends on its result. And how to use the results of the study of T-cell immunity in this context is still unclear.
I think that the main application of such complex methods, in relation to COVID-19, will be a detailed study of post-vaccination immunity, including an assessment of the state of the immune system in various immunodeficiency conditions, as well as the development of new methods for the prevention and treatment of coronavirus infection.
Interview conducted with the support of the Ministry of Science and Higher Education of the Russian Federation and the Russian Academy of Sciences.