Breast cancer is one of the most common types of cancer. According to the World Health Organization 2.2 million new cases of this disease were diagnosed in the world in 2020 alone.
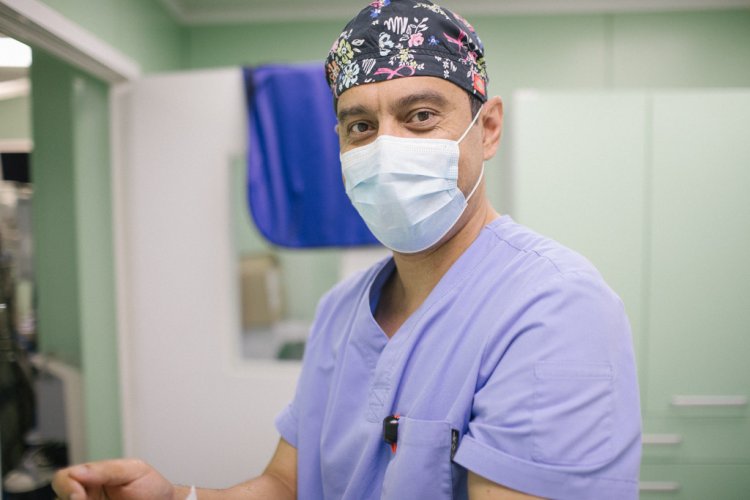
Scientific Russia discussed the risks of the disease, ways of its treatment and some methods of prevention under study with Aziz Zikiryakhodjaev, Doctor of Medical Sciences, Oncologist, the Head of the Department of Oncology and Reconstructive Plastic Surgery of the Breast and Skin of the P.A. Herzen – a branch of the Federal State Budgetary Institution “NMITs of Radiology” of the Ministry of Health of Russia.
Photo: Nikolay Mokhnachev / Scientific Russia
– Why does breast cancer occur more often than other types of cancer? Is this organ the most vulnerable?
– Breast cancer is truly the most common and at the same time the most studied disease in oncology. In Russia about 70 cases per 100,000 population are diagnosed every year, as a rule, it is diagnosed in elderly patients. Many factors and criteria influence the development of breast cancer. At the same time, this organ is not so developed in men, which makes women the most susceptible to the disease.
– Is breast cancer an acquired disease or is it inherent in the human body?
– About 20 years ago, everyone was sure that it was an acquired disease. At that time, the discoveries in genetics were only talked about, nobody had studied the genetic aspects of the disease seriously. Doctors clearly understood that the peak incidence of the disease occurred in women of old age: 55–65 years and older. It was believed that with age, every woman lived to see the problem of breast cancer, just as men lived to see prostate cancer. Therefore, the disease was thought to be acquired.
I remember my residency years – 1997–1998 – the whole institute was talking about a 40-year-old woman with breast cancer, they were saying that she was too young for this disease.
Later, the knowledge in the genetic field appeared. Then it was determined that there are genes, which mutations can cause this disease, so a conclusion was made that the disease among women who have cancer at a young age is related to genetic problems. Unfortunately, and surprisingly for me, we see young women of 22–25 years old who have this disease. Moreover, they have a more aggressive course of disease.
– Is it breast cancer that is getting younger or methods of diagnosis and research have improved?
– There are many theories about it. One of them says that we have lived the last few generations without any cataclysms: there were no major wars or epidemics. There were 2, 3, 4 generations, following each other, which could have transmitted genetic diseases. After the war, a generation of mutation carriers was lost, which means that this group of patients dropped out.
Today there is a theory that a third and fourth generation, which inherits these diseases from their parents, is emerging. It concerns not only breast cancer, but also other malignant tumors.
Photo: Nikolay Mokhnachev / Scientific Russia
Photo: Nikolay Mokhnachev / Scientific Russia
– Genetic changes that lead to the disease: what are these changes? As far as we know, foreign oncologists recommend preventive breast removal in case of certain changes in genes. What kind of studies are these?
– These questions are widely studied and discussed in the scientific community. The first one is: how can we prevent the development of the disease when a mutation, a break in the gene, is identified?
Unfortunately, today there is no pill that can be given to a patient to fix the break in the gene. There is the “Angelina Jolie effect,” who has been tested for these mutations. Then it was first stated that preventive mammary gland and ovarian removal was a possible way to prevent the disease. It encouraged the entire global scientific community to study the issue further.
About 10 to 15 percent of all patients carry the defect in the gene. It is believed that sooner or later they will develop breast cancer, some sooner, some later, but the older a woman gets, the higher the risk of getting the disease. If there is a break in the most common gene, the cumulative effect of the disease is seen by the age of 80 and reaches 60 percent. So, the question is – what do we do with these women? Do we have the right to offer a woman a preventive removal of the organ on both sides or should we detect the cancer at an early stage and ensure higher survival rates?
Patients have different opinions about it. I can tell you from my own practice: women who have had a tragedy in their family are more likely to agree to the surgery. If they have seen their mother or grandmother sick, if they share this tragedy with them, they are more likely to agree to a radical surgical treatment. Women who identify the mutation in themselves, but have not witnessed a similar story in the family, take the situation more philosophically: maybe the disease will not affect me, maybe there is no need to remove the mammary glands in advance?
There are two big studies of prevention in medicine today. The first is careful screening, observation of a patient who has been diagnosed with a mutation. This patient sees the doctor more often and they're examined more thoroughly, with special attention to mammary glands. There's also a problem with interval cancer – a disease that wasn't predicted can occur within six months between two examinations.
The second suggestion is the preventive removal of the mammary glands. This is more of a legal and ethical issue, because it is an aesthetically important organ for a woman. On the one hand, it is the prevention of a serious disease, but on the other hand, for example, in case of surgical failure or complications, a woman can become disabled, which can affect her psychological, emotional and social state.
– How does Russia's legal system look at preventive removal today?
– We've been discussing this issue for about 10 or 15 years. We have received the initial approval to preventive removal of one breast in women with mutations in the genes, in case the cancer has developed on one side. In that case, the contralateral breast can be removed preventively.
And the removal of two mammary glands without developed cancer is not legally supported in Russia today. The studies that we have conducted and the data that we have in the world literature do not yet represent a basis for us to offer women preventive bilateral mastectomy.
Some clinics perform mastectomies, calling them preventive. In fact, it is more of an aesthetic operation and has nothing to do with cancer prevention.
Photo: Nikolay Mokhnachev / Scientific Russia
– Nonetheless, are there any studies on preventive bilateral mastectomy going on in Russia? We have information that the first patient has already been operated upon. How are these studies going?
– Yes, we have initiated this kind of scientific research at the institute. We decided to see if what our foreign colleagues wrote was true – that 10 percent of patients with preventive breast removal without cancer diagnosis, have either precursors or the cancer itself detected during pathomorphological examination. Our colleagues from the United States claim that about 5 percent of patients who have had their glands preventively removed are found to have undiagnosed cancer.
We decided to do our own study and started to recruit a group of patients. We offer them a preventive bilateral mastectomy if they have a mutation and a severe family history. This is the group of patients who have a severe hereditary pathology in their family, i.e., a grandmother, aunt, or mother. We identify mutations in an extended or abbreviated genomic study and understand that sooner or later the patient will end up in a high-risk zone.
There are a lot of women who’d like to join the study, but we are very careful about the choice from a legal and scientific points of view. Some people, for example, can be pushed to have an organ removed because of fear of disease, but this is not an indication for surgery; there has to be some clear indications and criteria to be met. This protocol is designed precisely to develop these indications and to prevent the removal of an organ, for example, for beauty or aesthetic purposes.
We are constantly approached by women who have experienced tragedy in their families. Our mail is flooded, the call center is busy all the time.
– What stage of research are you at? How long can it take and what results can it bring? Can such surgeries eventually become routine?
– I hope that in the near future that group of patients at high risk for breast cancer will be included in this study. And in the future, there will be a group of patients directly targeted for this.
In some women, the fear of the disease is so high that they ask to have the organ removed before the diagnosis is confirmed, even without reconstruction of the gland. It happens, for example, when a woman had seen what happened to her mother and was told by a geneticist at a consultation that she was at high-risk of getting the disease, too. If we actually confirm in the study that the percentage of detected cases of cancer in preventively removed glands is quite high, for example 10 percent, then we would have the right to at least offer such an operation.
However, we clearly understand that based on the results of research, another method of prevention may emerge. Surgery is still a very aggressive, radical method, which may have its own complications. Patients need to understand that. First of all, when it comes to preventive mastectomy, we need to talk to the patient in terms of possible complications.
– How long do you plan to do the research?
– The protocol was launched in 2021 and will last for three years. We are now recruiting suitable volunteers for the study. In each case, we conduct a thorough genetic study before surgery, something that takes a long time. Typically, this is a complete genome sequencing, up to and including all pathomorphological and immunohistochemical studies.
Only when the scientific research is complete, we will reveal the statistics and talk about the results.
– How accessible are studies of genetic disorders in Russia today?
– Federal institutions throughout Russia, including early treatment clinics, do have such facilities and laboratories. Studies of the most common mutations are performed on a free-of-charge basis as part of the MHI. If they see that a woman is at risk for hereditary factors, but we do not find mutations in the most common genes, we offer full genome sequencing. There is a genetics institute that performs these studies for free, if there are any indications, or at the patient's expense, if there are no such indications.
Photo: Nikolay Mokhnachev / Scientific Russia
Photo: Nikolay Mokhnachev / Scientific Russia
– Are there any treatment methods for breast cancer that can be considered most effective? Such as radiation therapy, chemotherapy, medication therapy…
– Over the past 10 years, we have had completely new insights into breast cancer. We used to be guided only by the stage of the disease. They used to say, for example, that in the first and second stages we could only treat the patient surgically, without adding any chemical or hormonal therapy. Today there is an immunohistochemical classification, which allows to tailor treatment for each patient.
Now, even if a patient is in the first stage of the disease, we can recommend chemical or targeted therapy. There are some new drugs, new studies, new markers that allow us to approach each patient so personally that the prognosis will be based on a tailored complex treatment.
I can say that breast cancer is a systemic disease that can affect other organs as well. And modern oncology is more of a combined or complex treatment. It means that we have moved away from purely surgical or medication methods. Today, combinations of chemotherapy with immunotherapy, surgery, or targeted and radiation therapies bring very good results. For example, experts in the United States report that the survival rate in their country already exceeds the disease rate. This means that the majority of women who have been diagnosed with breast cancer are recovering.
– What is the average mortality rate from breast cancer?
– Every country has its own statistics. It all depends on the stage of the disease at which a woman seeks help. Over the last 10–15 years the diagnostic possibilities have increased to such an extent that nearly 20% of patients are diagnosed with cancer “in situ” – zero stage. We used to detect cancer “in situ” only in 1–3 percent of patients. Or, for example, the first and second stages of breast cancer: previously we talked about 30–40 percent, today it's 70–80 percent of identified diseases.
This determines the patient's prognosis and treatment policy, their survival rate. If a patient comes to us during first or second stage, and we treat them in time, then almost 90% of women successfully survive the five-year period, which is a statistical indicator in oncology. And for many we see 10, 15, and 20 years. Considering that these are mostly women in their fifties and sixties, imagine them living up to an old age safely after treatment.
– Speaking about the increase in early cancer detection – is it improved diagnostic methods or increased awareness?
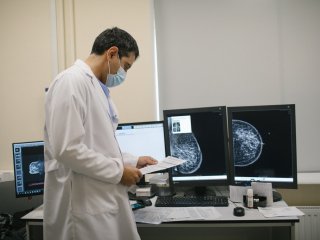
– That includes increased awareness, but mostly I would attribute it to the tremendous work that radiologists and mammologists do. Women need to pay attention to their health: no matter what their living conditions or social status are, they always have the possibility to have a mammogram at least once a year at their location.
A completely different kind of equipment has appeared. Digital mammographs, tomographs, and MRI machines can easily detect the tiniest tumors down to 0.5 cm and prove that this is the beginning of a malignant process. In the past, they could not be seen on native X-rays. In such cases, a single operation with hormone therapy, for example, may be sufficient. There is no need for complicated, heavy treatment with targeted drugs or chemotherapy.
– One of the trends in oncology is now called nuclear medicine. Are these developments somehow applied to the treatment of breast cancer?
– Regarding this question, we come back to the fact that cancer is a systemic disease that requires complex treatment. Today, it is no longer possible to cure a patient by surgery alone, because we try not only to remove the tumor, but also to return a woman to a healthy, normal life, meaning to perform an organ-preserving operation. Nowadays, surgery has evolved so much that by removing the tumor we can preserve aesthetics, restore beauty, and include radiation therapy in the treatment.
At this point, there is a need for devices that allow to irradiate the mammary gland without affecting other organs. Previously, radiation therapy involved irradiation of the lungs, heart, esophagus, and muscles. Today there are practically no contraindications, the devices are so selective that it is possible to irradiate the breast without affecting other organs, even in elderly women with certain pathologies, for example, a cardiac disease.
These are undoubted achievements in nuclear medicine, the emergence of proton accelerators, the enhancement of photon machines.
– What advice do you have for women regarding early detection of the disease? What could be a warning sign?
– There used to be a concept of self-examination. There was a lot of controversy about how effective it was and whether it could help a woman to identify a disease in time. However, it is certainly one of those methods that can help to draw attention to changes in the organ. Even a trivial change in the color of the skin or the appearance of any secretions from the nipple of the breast can be a reason to go to the experts.
Of course, in addition to this recommendation, all the criteria are clearly defined: at what age, to whom, and what examination is recommended. Ultrasound diagnostics is more common among young women, and mammography is more popular with the elderly. This is all specified in standard guidelines. There used to be an annual physical examination: doctors would come to an enterprise and do fluorography and mammography on everybody. Now it's partly returning, but it all depends on the person's attitude towards it.
Generally speaking, every woman should visit both a mammologist and a gynecologist at least once a year. This is especially relevant to women in the premenopausal and menopausal age, which accounts for the peak of disease incidence. These simple rules will help to detect and successfully treat the disease in time.
– To summarize: cancer can now be identified at an early stage, treatment is more effective, and prevention methods are being improved. So, it's not a death sentence as it was portrayed 20 years ago?
– It's not a sentence at all. I say these things even to those patients who are found to have disease processes at an advanced stage. Yes, there is a certain group of patients who do not respond well to certain therapies. But most of the world studies show that even patients with the third stage of the disease and patients with generalized forms of the disease and metastases in other organs can be treated and have positive results.
Let alone a two- or three-year survival rate, we are already talking about a 5–10-year criterion.
Photo: Nikolay Mokhnachev / Scientific Russia